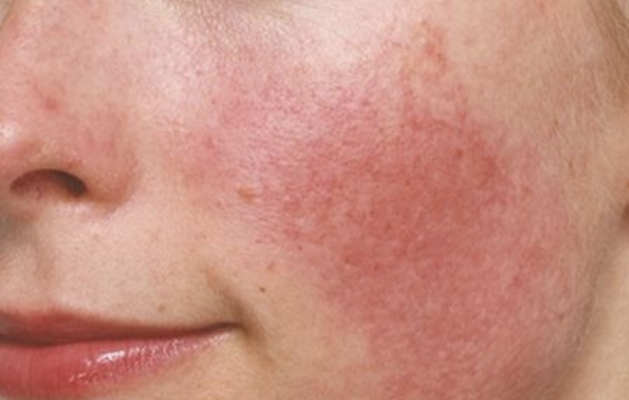
Have you ever noticed splotches of redness on your cheeks and the center of your face?
This may be visible after intense exercise or after certain meals. You may even notice significant redness after consuming alcohol.
A 2018 study by Dr. Jacob Thyssen and colleagues at the University of Copenhagen found that 415 million people worldwide currently suffer from rosacea. This chronic inflammatory skin condition leaves the skin on the face visibly red, and frequently warm, slightly swollen, and with inflamed blood vessels.
Patients are often confused and frustrated with the redness that appears on their skin, as rosacea is sometimes misdiagnosed, and acne-like pustules may form.
Understanding the cause of the inflammation allows our physicians to develop an accurate and effective treatment plan that will reduce visible flushing.
Understanding Rosacea vs. Redness
Unfortunately, rosacea is often confused with other skin conditions, given the symptomology and similar appearance on the skin.
To mitigate misdiagnosis, always be sure to check with a board-certified dermatologist to confirm the diagnosis.
Below, we’ve listed the top 5 conditions that cause facial redness, often misdiagnosed as rosacea, and how to better understand your skin for the best possible treatment.
#1 Atopic Dermatitis
Atopic dermatitis, also commonly referred to as eczema, refers to a chronic inflammation appearing as a recurrent, itchy, dry, flaking rash. When seen on the face, eczema may appear as cracking, red splotches visible on any part of the skin.
To the frustration of many patients, eczema recurs. Understanding the trigger for your eczema can help to prevent as many recurrences. The triggers can be grouped into 3 main areas:
- Skin barrier breakdown
- Inflammation
- Bacterial overgrowth on the skin
Irritants disrupt the skin barrier, which may trigger eczema flares. Common irritants include:
- Soaps and chemical cleansing agents
- Fragrances, perfumes & dyes
- Wheat, dairy, soy, and certain nuts
- Animal dander
A patch test may help you understand the trigger behind your eczema and offer advice on strengthening your skin barrier for reduced sensitivity and increased skin resilience.
A recent sickness, an allergic reaction, or stress can increase the level of inflammation on the skin, which leads to redness and could cause a flare.
#2 Psoriasis
Psoriasis looks very similar to rosacea, and the two are frequently confused during diagnosis.
With psoriasis, there is a rapid overproduction of new skin cells. There is a genetic predisposition, but certain causes can make psoriasis worse:
- Certain foods or medications
- Stress
- Cold, dry environmental conditions
- Lack of sunlight
- Hormonal imbalances
- Smoking
Psoriasis on the face appears similar to rosacea, but treatment options for psoriasis are very different. Certain medications used in the treatment for psoriasis, including topical creams and corticosteroids, may make rosacea worse. It is best to consult with one of our physicians to understand your diagnosis and develop an effective treatment plan.
#3 Lupus
Lupus is a chronic autoimmune disorder that can wreak havoc on the skin. Often, lupus will leave a butterfly-shaped rash across the nose and cheeks. Lupus can affect more than just the skin. Patients with lupus may experience rashes all over the body, chest pains, swollen joints, and extreme fatigue.
A board-certified physician can help you determine whether your redness and skin irritation is lupus or something else like eczema or psoriasis. Generally, patients with lupus have a rash visible on specific areas on each side of the nose and the upper lip.
Our physicians carefully assess your skin and perform biopsies to determine if lupus is the cause of your skin redness.
#4 Tinea (Ringworm)
Tinea, otherwise known as ringworm, is a fungal infection that can appear as a distinct “ring” pattern on the skin, setting it apart from the typical butterfly pattern of rosacea. Tinea is caused by a family of fungal species that live on a variety of surfaces, including:
- Bedding
- Clothing
- Towels and other linens
- Damp surfaces (for example, shower floors, especially of public showers)
- Pets
Teens and young adults are at a higher risk for developing ringworm, especially if living in a warm, humid climate. An accurate diagnosis must be made by a physician, and a biopsy may be necessary for optimal treatment.
#5 Menopause or Other Hormone-Related Triggers
Women in menopause typically experience hot flashes due to a significant drop in estrogen production. The link between estrogen and hot flashes is still unknown. However, it is suspected that the hypothalamus, which controls body temperature, may be affected by the hormonal changes.
Other hormone-related skin disorders that may cause redness in the skin may include:
- Cushing’s Syndrome
- Acne
- Hashimoto’s Thyroiditis and other autoimmune disorders
#6 Seborrheic Dermatitis
Seborrheic dermatitis is a chronic, widespread, but harmless skin condition. It can appear as flaky white scales with redness on the scalp and face. It is caused by a yeast that grows naturally on our skin. It eats the oil produced by our skin and hair. In certain patients, the yeast overgrows, causing redness and flaky white scales. The redness and irritation can cause itchiness, making it appear similar to rosacea.
There are common triggers that can cause seborrheic dermatitis to flare, which include:
- Heat
- Stress
- Age
Treatment Starts With an Accurate Diagnosis
There are a variety of conditions that may cause your skin to appear flushed and red. Receiving an accurate diagnosis from our physicians is the best way to initiate an effective treatment plan.
It is certainly possible for the redness to be a temporary concern when exercising or in hot/cold climates. However, if redness lasts more than 2 weeks, schedule an appointment to see us.


